What is teleradiology?
Teleradiology is the exchange of digital images such as x-rays, MRIs, and CT scans between healthcare providers in different locations through electronic communication for the purposes of diagnosis and consultation.
What is required to perform teleradiology?
To perform teleradiology in the U.S., physicians must meet licensing requirements to practice telemedicine in the state in which they are acquiring and interpreting the study.
The ACR Task Force on International Teleradiology notes that “Physicians performing teleradiology services must have training equivalent to those physician providers of imaging services at that health care institution receiving these services.” The task force also states teleradiologists must engage in ongoing learning throughout their career to maintain skills related to the work they perform.
What’s the difference between diagnostic vs. non-diagnostic monitors?
In the ACR–AAPM–SIIM Technical Standard for Electronic Practice of Medical Imaging, diagnostic monitors or displays are also known as primary interpretation displays while non-diagnostic displays are referred to as secondary displays. The standard identifies specific technical requirements important for the image quality of diagnostic monitors while non-diagnostic monitors do not require the same specifications. These technical specifications help ensure the correct spatial and contrast resolution of images that is necessary for accurate interpretation.
In their review article examining the impact of computer display performance on the quality of digital imaging, Butt, Mahoney, & Savage (2012) highlight that compliance to the Digital Imaging and Communications in Medicine (DICOM) Part 14 Greyscale Standard Display Function “standards is considered critical and represents the most important difference separating medical grade displays from standard or commercially available devices.”
To understand the difference between diagnostic monitors vs. non-diagnostic monitors or commercial off-the-shelf (COTS) monitors, it’s helpful to review the ACR–AAPM–SIIM–SPR Practice Parameter for Digital Radiography. In this document, equipment specifications for diagnostic monitors are outlined and adherence to these guidelines is “strongly recommended”.
This document identifies specific display characteristics diagnostic monitors should have to ensure high quality imaging. These characteristics include luminance response and pixel pitch and display size.
Luminance Response
Luminance refers to photon energy that reaches the eye and is controlled by 3 factors:
- Ambient luminance (Lamb) – This refers to the brightness still visible on the monitor when the power is off as a result of diffusely reflected light in the room. The practice parameter states, “The ambient luminance should be less than one-fourth of the luminance of the darkest gray level.”
- Minimum luminance (Lmin) – This requirement is important because the human eye adapts poorly to contrast in very dark areas. Hence, the practice parameter states “the luminance of the lowest gray value, Lmin, should not be extremely low. The minimum luminance including a component from ambient lighting, L’min = Lmin + Lamb, should be at least 1.0 cd/m2 for diagnostic interpretation, 1.2 cd/m2 for mammographic interpretation, and 0.8 cd/m2 for secondary displays.”
- Maximum luminance (Lmax) – The ability of the human eye to detect contrast characteristics of an image “depend on the ratio of L’max (the luminance for the maximum gray value including the component for ambient lighting) to L’min.” This is called the luminance ratio (LR) and isn’t the same as the contrast ratio monitor manufacturers often refer to.
According to the practice parameter, a LR of 350 is required. For adequate contrast, LR should always be greater than 250 but not much greater than 350 since the human eye can’t detect contrast at significantly higher LR levels. The practice parameter states “The L’max of diagnostic monitors used for interpretation should be at least 350 cd/m2 with an L’min of 1.0 cd/m2. For the interpretation of mammograms, L’max should be at least 420 cd/m2 with an L’min of 1.2 cd/m2.”
Pixel Pitch and Display Size
Pixel pitch refers to the spacing of pixel structures and determines the amount of detail that can be shown on the display. While it’s common to see monitors classified by the number of pixels they display, the practice parameter recommends selecting diagnostic monitors based on pixel pitch and display size. A pixel pitch of approximately 0.200 mm and not larger than 0.210 mm is recommended.
When considering display size, it’s important to be aware that the viewer’s vision extends to the edges of the display due to peripheral vision. Therefore, it’s recommended that the diagonal display distance be approximately 80% of the viewing distance. The document explains “At 2/3 meter, this corresponds to a diagonal size of 53 cm (21 inches). Monitors with a pixel array size of 1,500 × 2,000 and a pixel pitch of 0.210 will have a diagonal size of 52.5 cm.”
This document also outlines other important display elements for diagnostic monitors that should also be considered such as several workstation characteristics and ergonomic factors important to radiological imaging.
In short, using a non-diagnostic monitor to make a diagnosis may result in diagnostic error and doesn’t meet the guidelines set out in the practice parameter.
Examples of Diagnosis Gone Wrong
Miller & Zois state about 31% of all practicing radiologists will be sued for malpractice at least once during their career. 75% of these malpractice lawsuits have “diagnostic error” or “failure to diagnose” as their basis. In addition, they note that radiology has one of the highest rates of malpractice in medicine.
 Painter shares the following case of a neuroradiologist who faced a lawsuit related to work she performed at home:
Painter shares the following case of a neuroradiologist who faced a lawsuit related to work she performed at home:
- • A male patient was admitted to the ER with a “severe, unrelenting headache that had been going on for a few days.” A CT scan without contrast was done and sent for interpretation to a neuroradiologist working from home. The only clinical information provided was “headache with dizziness and giddiness”. However, the ER physician testified this wasn’t completely accurate for the patient but was the closest option on the pull-down menu in the hospital’s electronic medical record system. The ER doctor testified the “real reason” he ordered the CT scan was to check for signs of a stroke or other cerebrovascular abnormalities. The neuroradiologist said she thought she saw artifact on the CT scan at home but did not recommend repeating the CT scan because of this concern nor did she recommend an MRI which provides higher resolution to assist in diagnosis. She also did not phone the ER physician to obtain more information. She interpreted the CT scan as normal. The patient was discharged from the ER that day and suffered a massive stroke shortly thereafter.
Miller & Zois provide the following example of a lawsuit against a radiologist group.
- • A 56-year-old female has a diagnostic mammogram that is interpreted as normal. A subsequent mammogram the following year shows she has a large tumor that results in a diagnosis of breast cancer. However, by that time, the cancer has spread outside of the breast and she dies two years after she is diagnosed. Her family sues the radiologist group for negligence in failing to identify the tumor during the first mammogram. The case goes to trial and the family are awarded $2.5 million in damages.
In Error and discrepancy in radiology: inevitable or avoidable?, Brady (2017) states “errors will always happen, but some can be avoided”. The question is “Which errors can be avoided?”
To answer this, Bruno, Walker, & Abujudeh (2015) suggest safety and quality in medical care may be improved considerably by reducing the variability in radiological processes. For example, this may be done by standardizing radiologists’ approach or the diagnostic imaging protocol. They also point out improvements to processes within systems of care are believed to contribute to fewer diagnostic errors.
Benefits to moving to diagnostic workstations for all radiology employees
Studies have shown improved accuracy as well as higher physician confidence with image interpretation using diagnostic monitors compared to COTS. This results in faster interpretation and diagnosis saving time and money while reducing the potential for litigation due to diagnostic error or failure to diagnose.
Although a more costly initial investment, medical grade monitors often prove their worth with ease of use, better quality images, and significantly longer life spans than non-diagnostic monitors that must be replaced up to four times more often than medical diagnostic monitors.
The ACR–AAPM–SIIM Technical Standard for Electronic Practice of Medical Imaging states consistent image presentation at workstations is essential for:
- • Technologists acquiring images
- • Radiologists interpreting images
- • Physicians using imaging to provide patient care
Consistent image presentation on diagnostic monitors combined with the most current workstation characteristics and ergonomics set out in the standard enable all radiology employees to do their best work.
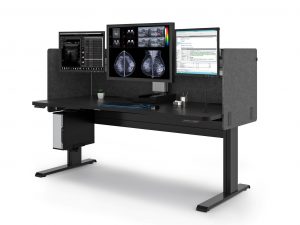
Working with Double Black Imaging to create the perfect radiology workstation
Double Black Imaging is an industry leader producing technologically advanced medical display systems that meet the high-quality standards radiologists have come to trust and rely on to provide accurate and timely diagnosis.
For information about quality medical grade displays, efficient workstations, the use of automated calibration tools and other benefits of purchasing monitors from Double Black Imaging, please contact our diagnostic imaging experts. We can answer your questions, provide demos, and show you how our monitors outperform those of the competition.
Contact our diagnostic imaging experts today to discuss your radiology department requirements.
Sources List:
https://www.cozen.com/templates/media/files/publications/tpl1604-hodge3.pdf
https://www.acr.org/Advocacy-and-Economics/State-Issues/Licensure-Requirements
https://www.acr.org/Practice-Management-Quality-Informatics/Legal-Practices/Teleradiology
https://www.acr.org/-/media/ACR/Files/Practice-Parameters/Elec-Practice-MedImag.pdf
https://onlinelibrary.wiley.com/doi/full/10.1111/j.1834-7819.2011.01660.x
https://www.acr.org/-/media/ACR/Files/Practice-Parameters/rad-digital.pdf?la=en
https://otechimg.com/publications/pdf/wp_medical_image_monitors.pdf
https://www.millerandzois.com/malpractice-lawsuits-against-radiologists.html
https://www.painterfirm.com/a/730/Three-mistakes-radiologists-make-when-reading-a-CT-MRI-or-scan
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5265198/
https://pubs.rsna.org/doi/full/10.1148/rg.2015150023
https://www.itnonline.com/article/consumer-grade-vs-medical-grade-displays