Load balancing, or equitable distribution of radiology workflow, has been a longstanding and widely disputed issue in radiology stemming back to the pre-PACS era. Unequal workloads resulting in unequal compensation have threatened to divide many imaging practices. The introduction of PACS solved many of the imaging and reading problems radiologists used to face, and even saw some groups doubling production, but did not fill in all the gaps in radiology workflow.
The advent of PACS also occurred during a period of healthcare reform that demanded higher production and higher quality benchmarks while lowering reimbursements. And new problems emerged as easier cases were quickly processed while complex cases sat unattended on work lists for days. This has resulted in a full circle return to unequal workload distribution and conflict among radiologists.
Why Is Good Radiology Workflow Important?
Balanced medical imaging workflow is an elusive goal radiologists have pursued for decades due to its widespread effects on both the profession and the healthcare system. And while a radiology practice or department completes many tasks, a study has shown that roughly 80% of radiology workflow problems can be attributed to 20% of its cases. Identifying these problems can help bring about customized solutions.
With radiology being a $100-billion dollar industry, leaders in the field point out “approximately $15 billion to $20 billion of radiology’s expenditures are unnecessary and avoidable. Either the right test is conducted at the wrong time, or patients receive a repeat exam. Regardless, improving workflow can save not only money, but it can also save practices’ and departments’ time.”
Besides saving money, more efficient workflows can help reduce delays in patient care as well as medical record and clinical errors. This can be accomplished through real-time communication to manage and transfer patient data.
Another gap in radiology workflow as a result of the evolution of imaging technology is communication between radiologists and clinicians. It used to be that clinicians had to call and speak to the radiologist about imaging results or physically walk over to the radiology department to discuss and view patient results. Since the introduction of PACS, clinicians can review radiological reports and images anytime from any location. While the importance of face-to-face communication may be debatable, the importance of accurate and timely communication between radiologists and clinicians for patient safety and care remains important to all physicians.
Improved imaging and workflow efficiency also results in better patient care as a result of improved consistency, higher quality imaging, and individualized medical care.
Better working relationships with care providers and more effective use of office hours are other important benefits when radiology workflow is handled efficiently and fairly distributed.
How Has Technology Changed in Radiology?
It is now common to see health systems with different PACS installations from different vendors spread across the networks of imaging centers and hospitals. A shared goal in these systems is to aim for equitable case distribution amongst radiologists across these vast networks, and to try to improve efficiency and workload balance while ensuring the most qualified radiologists are assigned the most complex cases.
Brady concurs, explaining “Orchestrating workflow more efficiently is a win-win-win for patients, physicians, and staff. Patients benefit when the radiologist who’s best equipped for and experienced in reading that type of subspecialized exam is automatically chosen to read it, and it’s routed quickly and efficiently.”
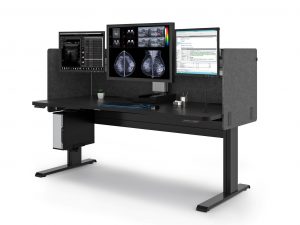
One of the medical imaging workflow problems Double Black Imaging solved is requiring different displays depending on the modality being read. It is not conducive to a smooth workflow if a radiologist has to change workstations to read CT,MR, Nuc Med, Chest, Bone or Mammo/Tomo. Their 8MP and 12MP large format displays enable doctors to read any modality from one large screen. 5MP Color displays provide radiologists a dual monitor set up for multi-modality imaging if two screens are preferred over one.
How Has Technology Changed Medical Imaging Workflow?
To help improve communication between radiologists and clinicians, some radiology departments have found unique ways to use imaging technology. For example, NYU Langone Medical Center in New York City has incorporated virtual radiology rounds and multimedia reporting to improve communication with clinicians.
For virtual radiology rounds, clinicians arrange online meetings with radiologists to review images and reports. “The clinicians and radiologists then use web cameras to see each other during the meetings, and they also remotely share a computer screen and mouse. This allows both parties to point out details on the images, provide feedback, and ask questions — just as they would during in-person consultations….” Not only has this improved communication with clinicians, but radiologists also feel it makes them more “visible” and helps create greater value for patients and referring physicians.
Due to the success of these virtual rounds, radiologists at NYU Langone plan to begin offering virtual consults on demand to physicians’ offices at hospital outpatient departments as well. When the clinician loads the images into the hospital’s PACS, a message will pop up asking them if they want to speak to a radiologist. If the clinician clicks ‘yes’, the radiologist assigned to those cases receives a message on their phone or other electronic device advising them an on-demand consult is being requested. Radiologists at NYU Langone anticipate this service will provide significant value to both physicians and patients while restoring the role of radiologists as consultants and integral members of the clinical care team.
What Impact Will AI and Machine Learning Have on Radiology?
Artificial intelligence, also known as machine intelligence, refers to a wide scope of intelligent functions that can be performed by computers such as planning, language processing, knowledge representation, problem solving, and actual “learning” based on previous data it has reviewed and processed.
While AI is not expected to replace radiologists, it has been compared to the autopilot function on airplanes that relieves pilots of performing repetitive and tedious but necessary safety checks and tasks. Arazi notes that once the COVID-19 pandemic tapers off, AI will play a key role in helping radiologists save lives post-pandemic. He suggests it will do this by helping prioritize growing numbers of non-urgent but important procedures that were set aside due to the pandemic, such as cardiovascular imaging, bone-health scans, and mammography screening.
AI also has the potential to change the role of radiologists from active disease diagnosticians to proactive diagnosticians, assisting patients with early intervention and even preventive care by identifying potential problems before they occur.
Similarly, machine learning is one type of artificial intelligence that can be used to pull, organize, and analyze information from big data sets created by large electronic medical record systems. This information can then be used as a basis for anticipating patient outcomes and clinical decision-making.
In the future, machine learning may also help improve different components of radiology workflow such as radiology reporting, postprocessing and dose estimation, triaging, order scheduling, quality control of exams, detection and interpretation of findings, and support systems for clinical decision-making.
For all your radiology imaging needs, including innovative software solutions and superior medical-grade displays, contact our diagnostic imaging experts at Double Black Imaging. Our unparalleled customer service and highly knowledgeable staff set us apart from the competition, making us the first choice for all your imaging needs.
Source List:
https://www.radiologytoday.net/archive/rt0220p8.shtml
https://www.jacr.org/article/S1546-1440(18)30257-6/fulltext
https://www.diagnosticimaging.com/view/how-streamline-radiology-workflow
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6650448/
https://www.acr.org/Practice-Management-Quality-Informatics/Imaging-3/Case-Studies/Information-Technology/Closing-the-Gap
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6542626/
https://www.weforum.org/agenda/2020/10/how-ai-will-change-how-radiologists-work/